Resources
Special Initiatives

Stories (21)
“Maybe I am the lucky one”
A spontaneous HIV test that yielded a positive result changed Martha Clara Nakato’s life forever. When Ms Nakato, who lives in Uganda, found out she was living with HIV, she was 14 years old and had never had sex.
“I accompanied my twin brother only to support him to take up the test. I didn’t know taking one too would change my life forever,” she says as she recalls her shock and confusion at her result.
Her brother’s HIV test came out negative.
Ms Nakato soon discovered from her father that she was born with HIV. She is the only one of her eight siblings who contracted HIV from her mother. She lost her mother to AIDS-related illnesses when she was just five years old.
“I don't know why this had to happen to me. Maybe I was the lucky one; maybe there was a purpose meant for me. When I look back, I now know the only way you can find your purpose in life is to think about that one thing that hurt you the most,” Ms Nakato says.
Ms Nakato has transformed her pain to power and works as a human rights defender and HIV advocate with the Uganda Network of Young People Living with HIV/AIDS (UNYPA).
In 2019, she was recognized as one of the Global Fund to Fight AIDS, Tuberculosis and Malaria’s five faces that championed the worldwide sixth replenishment campaign.
“I do a lot of mentorship and motivational speaking,” says Ms Nakato, who uses her own story to demonstrate how adherence to HIV treatment can help people living with HIV live a full and healthy life.
Much of Ms Nakato’s advocacy and mentorship involves interacting with young people in their communities with in-person dialogue. Following the COVID-19 outbreak, she had to rethink how to reach young people while adhering to the social distancing measures that followed because of the pandemic.
“Most of those engagements that involved face-to-face were not able to happen. Looking at young people in the rural areas who don’t have access to the Internet or a smartphone, we really had challenges reaching out to them,” Ms Nakato says.
However, Ms Nakato and her team realized the importance of reaching out to young people on social media platforms, such as Facebook, to get her message across.
UNAIDS provides financial and technical support to the annual Y+ beauty pageant and youth summit, events that are organized by UNYPA. The pageant crowns a Mr and Miss Y+, encouraging young people living with HIV to come together, celebrate their beauty and address HIV-related stigma and discrimination.
During the COVID-19 outbreak, UNAIDS ensured that community-based organizations such as UNYPA had access to national platforms—for instance, the national COVID-19 national secretariat—so that organizations could engage in dialogue with the government and thereby provide better relief and food support to communities in need.
Ms Nakato was born in 1996, a time when HIV treatment was inaccessible in Uganda. In that year alone, 34 000 children between the ages of 0 and 14 years acquired HIV.
Today, 95% of women living with HIV in Uganda have access to services to prevent vertical (mother-to-child) transmission of HIV. There has been a significant drop in vertical transmission and the country has achieved an 86% reduction in HIV infections among children since 2009.
“I don’t want to give birth to a child who is HIV-positive or see any other young woman do so. We now have the power to prevent this from happening, not like many people in the past who didn’t have that chance,” she says.
As an AIDS activist, Ms Nakato has plans for herself and society, hoping to see an AIDS-free world. She stresses the importance of adhering to HIV treatment to help make that a reality.
“One thing I know is that I am the proof of treatment. I am proof of what self-love is,” she says.
Challenge the stigma, pursue your right to health
Adolescent girls and young women must boldly and unapologetically seek sexual and reproductive health and rights information and services. The stigma and harmful gender norms associated with sexual and reproductive health and rights are not going anywhere, says Nyasha Phanisa Sithole, a Zimbabwean sexual and reproductive health and rights leader.
“If you are afraid of stigma, then you will not be able to access these services because we are not going to have a stigma-free environment any time soon,” she says.
Working as a sexual and reproductive health and rights advocate and a regional lead for young women’s advocacy, leadership and training at the Athena Network, Ms Sithole believes everyone has a role to play in changing the status quo and influencing decision-making.
“My story is common. It is that of a 16-year-old adolescent girl who needed access to HIV prevention commodities, but only had condoms available and, in rare cases, pre-exposure prophylaxis,” Ms Sithole says, reflecting on her experience as an adolescent.
Despite this common story, the need for comprehensive HIV, sexual and reproductive health and rights and sexual and gender-based violence services in the eastern and southern African region is critical.
Adolescent girls and young women aged 15–24 years account for 29% of new HIV infections among adults aged 15 years and older in the eastern and southern African region, when they only comprise 10% of the population. This means that there are 3600 new HIV infections per week among adolescent girls and young women in the region, which is more than double that of their male peers (1700 weekly).
The stigma and discrimination that young people face, particularly adolescent girls and young women, to access sexual and reproductive health and rights services creates barriers at various levels, including the individual, interpersonal, community and societal levels.
Furthermore, documented health rights abuses include the unauthorized disclosure of health status, being denied sexual and reproductive health and rights services and related psychological violence.
In 2014, Ms Sithole went undercover as a secret client at a youth-friendly health centre in Harare, Zimbabwe’s capital city, in a district with residential areas and schools. The first person she encountered at the centre was a nosy security guard.
“He asked me: ‘What do you need?’ A health screening, I replied. Then he asked, “Asi wakarumwa?” Meaning, “Have you been bitten?” In Shona, this is street language for someone who has a sexually transmitted infection,” she recalls.
Had she not been well-informed, Ms Sithole says she would have felt scared. “It’s something that can scare you or put you off to say, “It’s just a security guard, why are they mocking me or my situation?” Because imagine if I really had a condition that I wanted to manage, what would happen then?”
Ms Sithole said health-care workers sometimes look at adolescent girls and young women accessing sexual and reproductive health and rights services with disdain and judgement and ask, “How old are you and what do you need the condom or contraception for?”
Considering the stigma attached to accessing sexual and reproductive health and rights services, community organizations play a critical role for adolescent girls and young women. Organizations empower them with sexual and reproductive health and rights information and service referrals.
However, COVID-19 greatly impacted how these organizations work in Zimbabwe, which enforced lockdown restrictions to curb the spread of the virus.
“I think all governments weren’t fair when they clamped down restrictions on each and every organization that was working in communities,” Ms Sithole says, adding that it negatively impacted young people’s access to sexual and reproductive health and rights services.
To mitigate these risks, the Global HIV Prevention Coalition, co-convened by UNAIDS and the United Nations Population Fund, came on board to provide financial and technical support to the Athena Network in 10 countries, including Zimbabwe, to establish What Girls Want focal people in each country. During the COVID-19 pandemic, the focal people, who are adolescent girls and young women, mobilized their peers to conduct dialogues via WhatsApp to discuss the issues they face and seek peer support.
Ms Sithole says governments should invest in policy change and development to create an enabling environment where adolescent girls and young women can access sexual and reproductive health and rights and HIV information and services.
Despite the stigma and discrimination attached to seeking sexual and reproductive health and rights services, Ms Sithole says adolescent girls and young women should realize their power and use their agency to get what they need.
“Think about your life because your life is more important than anything else. So, no matter what happens, if you know there is a service you can access, go for it,” she advises.
Phenomenal Positive Youths are young people living positively with HIV, working towards the elimination of stigma and discrimination, adherence to HIV treatment, access to sexual and reproductive health and rights services and mental health support in Zambia.
UNAIDS has facilitated sexual and reproductive health and rights training for the Lusaka team of Phenomenal Positive Youths and plans to extend it to other districts in Zambia. The training will now include the impact of the COVID-19 outbreak on young people living with HIV, which is currently being evaluated through an impact assessment survey.
Currently, its members are part of the multisectoral risk communication community engagement pillar, as recommended by the World Health Organization’s COVID-19 Strategic Preparedness and Response Plan. Under this pillar, they are involved in creating and disseminating messages on COVID-19, busting myths, social listening and raising awareness, under the guidance of the Ministry of Health in Zambia.
UNAIDS has advocated for the implementation of multimonth dispensing of HIV treatment in Zambia. As a result, the Ministry of Health has issued a national circular to accelerate the implementation of the multimonth dispensing policy, instructing health facilities to provide three to six months of antiretroviral medicines to people living with HIV. Phenomenal Positive Youths is encouraging its members and health-care workers to follow the new guidelines.
While the policy is being implemented, Oswald Chisenga, the team leader of Phenomenal Positive Youths, said the organization has noticed that young people have experienced challenges in accessing their monthly supply of HIV treatment. “The limitation of travel during the COVID-19 outbreak, the fear of exposure to the coronavirus and the associated stigma is restricting people from visiting health-care facilities, even with the revised national guidelines,” he said. “Even messages on COVID-19 have been misinterpreted by people as meaning they should not go to a health facility, even when the need arises.”
Thus, the organization has developed an unconventional and innovative approach to ensure that its members have an ongoing supply of antiretroviral therapy, called chilimba (a commonly used local word meaning to loan or advance a colleague something). Members of the organization loan their antiretroviral medicines to one another until the person in need can obtain their supply, at which time the medication is returned.
“We help each other so that no one skips a day or does not have enough antiretroviral therapy due to different circumstances. It may be because of illness, or the person is very far from the health facility or they have no documentation to access the health facility,” said Mr Chisenga. “We communicate with one another using our social media groups. This helps us to maintain adherence, encourages openness and virtual interactions or physical ones while observing social distancing guidelines,” he added.
This is only one of the innovations that Phenomenal Positive Youth has brought into the youth-led movement in Zambia. The group was also among the first associations to speak openly about mental health among young people, especially among young key populations and young vulnerable people.
Sex work during COVID-19 in Tanzania
“After COVID-19 kicked in, it has been too difficult to get customers,” says Teddy Francis John, a sex worker from Zanzibar. Since the outbreak of COVID-19, she has faced increased difficulties to earn an income to provide for herself and her two children.
“Everything has become tough and I had to start a small business of selling alcohol—local brew,” she says. The business also helps her meet new clients, as they come to her for drinks and are less vigilant about social distancing guidelines.
Ms John used to live and work in Zanzibar town, but to better earn an income and avoid paying rent, she decided to move to a more rural area. Here, she says, she can more easily find new customers for her local brew.
Rehema Peter is facing a similar situation, just on the other side of the ocean on Tanzania Mainland. She lives in the crowded suburb of Temeke in Dar es Salaam and works as a sex worker and volunteers as a peer counsellor for people living with HIV and for people who use drugs.
Her clients were regulars who used to come to her house, or she would visit those she could trust in their homes. But when COVID-19 broke out, they stopped coming.
“Coronavirus made life very hard. Payment at work used to be little and when COVID-19 came it reinforced the situation. On the side of my partners [clients], they stopped visiting and calling me. The very few who used to visit me often, I called them, but they said they have no money because of COVID-19, as some stopped going to their jobs,” says Ms Peter.
At her job as a peer counsellor she was offered fewer shifts, meaning a lower income. Because she is a former drug user, she has received some support through the Tanzania Network for People who Use Drugs (TaNPUD), which has been supported by UNAIDS to distribute food and hygiene items to people who currently use drugs and people in recovery.
“I just try to be calm and find other means [of income]. I’m searching for additional organizations that can help or support me anyhow. I also try to prepare soap and oil from the knowledge that TaNPUD gave me and I sell it,” says Ms Peter.
Continued services
Both Ms Peter and Ms John are living with HIV and are on HIV treatment. Due to the advocacy and assistance of UNAIDS and other partners of the Tanzanian government, disruptions to HIV services have been minimal in the country. This is felt by both women.
“During this time, it has become difficult to get services in government health facilities; unless you go to a private hospital where you must have cash. However, there is no problem at all in getting HIV-related services, including my treatment,” says Ms John.
Ms Peter say she can now get three months multi-month dispensing of antiretroviral treatment—even up to six months—since the healthcare staff do not want congestion in the clinics. This has helped both women in adhering to their treatment.
Increased stigma
Both Ms Peter and Ms John have experienced an in increase in the stigma and social exclusion they also face as sex workers and as women living with HIV during the COVID-19 outbreak.
“As some people know that I am living with HIV, they tease me. They say ‘prepare yourself for death. People like you never heal. You must prepare for your final journey’” recounts Ms Peter. She has faced discrimination in the community, but her family stands by her.
Ms John also faced increased gossip and mocking of her because of her work.
“People in my surrounding communities started mocking me and others. They gossiped as to how I would earn a living as there are not going to be customers because of the COVID-19 outbreak.” Says Francis John
Despite the COVID-19 outbreak being declared over in Tanzania and despite their continued efforts to find other means of livelihood, earning an income is still hard for the two women, due to continued social distancing regulations.
“[It] has been very difficult to provide this service and this harmed us economically. I know COVID-19 has affected the whole world but it has affected sex workers more because of the nature of our services; it involves proximity,” says Ms John.
Adrian Jjuuko heads up the team at Human Rights Awareness and Promotion Forum (HRAPF) in Kampala, Uganda.
He is the dictionary definition of an ally—a heterosexual lawyer who defends people who live on the margins of Ugandan society: lesbian, gay, bisexual, transgender and intersex (LGBTI) people, sex workers, refugees, people who use drugs and women who are survivors of domestic violence.
Mr Jjuuko founded HRAPF in 2008 to create awareness of human rights and provide legal support to marginalized people, mostly members of the LGBTI community.
“This is not the favoured job of a lawyer in Uganda,” he laughed. “When young graduates come out of law school, most would choose commercial litigation. I chose this. I chose it because I love it,” he added.
HRAPF started out as an organization that represented marginalized people but increasingly took on cases from members of the LGBTI community. Mr Jjuuko said that this is because, in Uganda, LGBTI people “are generally not treated like citizens with rights—not by law, culture or religion.”
Because of the stigma around the work that HRAPF does, “other lawyers don’t think we are real lawyers,” said Mr Jjuuko. “You live with the professional discrimination,” he sighed.
Uganda is one of 13 countries in the eastern and southern African region that criminalizes same-sex sexual relations. Under the Penal Code, “carnal knowledge against the order of nature” between two males carries a potential penalty of life imprisonment.
Evidence shows that the more marginalized, stigmatized and criminalized people are, the higher their vulnerability to HIV and violence.
Roughly one quarter of the 580 000 new HIV infections in the region in 2019 were among key populations and their sexual partners.
In sub-Saharan Africa, one in three transgender women have been attacked and 28% raped at least once in their life.
HRAPF represented the 14 gay men, two bisexual men and four transgender women (known as the COSF20) who were arrested in late March 2020 when police raided the Children of the Sun Foundation premises, an LGBTI shelter on the outskirts of Kampala. They were between the ages of 18 and 25 years and had been thrown out of their homes because of their sexual orientation and/or gender identify.
Police said the young people were violating social distancing rules that banned gatherings of more than 10 people in public spaces, restrictions imposed due to the lockdown in response to the COVID-19 outbreak.
However, they were not in a public place, but the place they called home.
Mr Jjuuko said this is one of many cases where COVID-19 restrictions are being used to violate human rights. The young people were arrested on the site on the suspicion of homosexuality and the charge was later changed at the police station to take advantage of the government restrictions.
It took Mr Jjuuko and his colleagues 43 days of applications, letters, meetings and court dates for HRAPF to be granted access to their clients; another two to actually see them; another five to get the charges dropped and the first 19 released, and yet another seven days for the final detainee to be released.
Mr Jjuuko and his colleagues had to hitch rides on cargo trucks en route to the prison, and use motorbikes and bicycles, to access their clients because of the restrictions placed on the operation of motor vehicles during the lockdown.
During the 50 days they spent in jail, the young people were subjected to gross human rights violations, such as beatings with wire, burning with pieces of firewood between their thighs, and, in one instance, an anal examination in a bid to “prove” homosexuality.
This is not the end, said Mr Jjuuko. HRAPF wants the prison authorities to dismiss the staff who perpetrated the violations and damages paid to the young men and women.
HRAPF’s work has turned from legal aid to humanitarian assistance, said Mr Jjuuko. The young people need food. A place to stay. It’s not enough to get them out of jail when they have no means and nowhere to go.
“The reason we do this is because no one else is doing it. There are basically no other legal aid service providers for LGBTI people. That is a feeling of contribution that you can’t take away.”
COVID-19 has made things even more difficult.
“We all need to come together and fight COVID-19 but we must not forget about marginalization and discrimination. How can we tailor our support to marginalized people? How do we protect people’s rights … think about people who need access to medicine and people who can’t use public transport? We need to think about the multiple dimensions of vulnerability,” he said.
UNAIDS continues to support the work of HRAPF to advance human rights and the right to health among key populations in Uganda. In 2020, it provided technical and financial support for a six-month project, which included sensitization meetings on HIV and human rights for key population groups from civil society, including information on the provision of free legal services to members of the community who are detained.
On the consequences of his work on his life, Mr Jjuuko shrugged and said, “It doesn’t matter. You just learn to live with it.” And in the same breath, he added,” As a lawyer, you must fight like a gladiator for your client to be protected.”
Community-based organizations in Dar es Salaam, United Republic of Tanzania, with assistance from UNAIDS, are supporting women who use drugs and their families to survive during these difficult times.
“Before the pandemic, life was simple and better. I used to do activities at the beach, such as cleaning fish, helping people load and clean their boats, and they would pay me. I would help my daughter wash her clothes; I would escort her to school and cook food for her. Life was simple,” said Doroth Hassan as she sits in the office of SALVAGE, a sister organization of the Tanzania Network for People who Use Drugs (TaNPUD), in Kigamboni, Dar es Salaam.
Ms Hassan would normally provide for herself and her daughter by doing sex work and other informal jobs, such as the work on the beach. But this has become a challenge since the onset of the COVID-19 pandemic.
“Now life has changed. I live in fear and worry. People who I worked for don’t want to pay, with the excuse that they have no cash because of the coronavirus. Everything changed. Life is tough. Clients disappeared, vanished. And the few who are still coming cheat; they pay less for sex,” said Ms Hassan.
She is not alone in her worry. Most of the women who use drugs in Dar es Salaam survive in the same way as Ms Hassan does, by doing sex work, trading and doing other jobs in the informal sector. They live in camps for people who use drugs or in informal and densely populated settlements.
With support from UNAIDS and other partners, local community-based organizations, including TaNPUD and SALVAGE, have been able to provide some relief to women in the camps and settlements in Dar es Salaam.
“TaNPUD raised awareness and SALVAGE provided buckets, soap and food with other hygiene materials to us and other women in the community. TaNPUD always advocates for our health rights,” said Oliver Kinanda, a person who previously used drugs and is now on opioid substitution therapy.
Ms Kinanda also volunteers at the Medication-Assisted Treatment (MAT) clinic in Temeke, where she lives. Here, she informs people on prevention of tuberculosis (TB) and takes samples from clients for TB screening. With the onset of COVID-19, however, her tasks have shifted.
“As a peer educator I have knowledge of prevention of COVID-19 and provide education and awareness. Together with other people who use drugs I also got help; for example, face masks,” said Ms Kinanda. She has also received information and support from other local community-based organizations, including donations to the community and the clients she works with in the Temeke MAT clinic.
Ms Hassan received the same support.
“TaNPUD is raising a voice on our behalf, and SALVAGE, as the sister organization of TaNPUD, supporting women, has been linking us to care and treatment with other services and providing shelter, food and hygiene support to us,” she said.
The support, distributed with financial and material assistance from UNAIDS, will help to alleviate some of the consequences of the global pandemic, even as the effects of COVID-19 are slowly wearing off in the United Republic of Tanzania.
Happy Assan, the Coordinator of TaNPUD, said this support has so far reached 55 families of women who use drugs in Dar es Salaam.
“The support covered food and hygiene needs. It also provided women with the ability to stay at home instead of going out, for example to do sex work, and to negotiate less risky sex. The support reduced fear and worry about meeting the food needs of families with children,” said Ms Assan.
Many of the women who use drugs are living with or at risk of HIV infection and depend on reliable access to treatment and care, including harm reduction services. Despite the support in the community, some services that the women who use drugs depend on have been halted.
“Harm reduction services have been interrupted; they are less. No condom distribution or other commodities, only needle and syringes distribution. At least now SALVAGE is helping with sanitary items. At hospital there is no other support; HIV treatment only,” explained Ms Hassan.
Ms Hassan and Ms Kinanda both recount facing increased stigma during the pandemic—some derived from unintended consequences of the support, since the face masks they received were a certain colour, making the wearer identifiable in the local community as a person who uses drugs. Stigma and discrimination at hospitals is also reportedly high, adding to the difficulties of accessing services. But most difficult is the financial loss because of the pandemic.
As Ms Kinanda puts it, “No clients, no pay. Financially it is hard because my clients say they have no cash because the coronavirus has affected their jobs. I continue providing awareness and education to the community and my family too. I financially suffer, but what can I do other than continue pushing on?”
The COVID-19 pandemic and women living with HIV: Caroline Damiani
Unlike many other countries in the region and the world, no lockdown measures were put in place at the height of the COVID-19 pandemic in the United Republic of Tanzania. In June, all restrictions on movement and gatherings were lifted. Nevertheless, the restrictions impacted people’s health and livelihoods, especially those who work in the informal sector, most of whom are women.
Women such as Caroline Damiani, from Chamazi, an administrative ward in the Temeke district of Dar es Salaam.
While, according to the government, about 83% of the 1.7 million people living with HIV in the United Republic of Tanzania are on HIV treatment, this leaves around 300 000 people living with HIV vulnerable. It has been shown that people with underlying health conditions are more susceptible to severe COVID-19 disease.
Thus, COVID-19 is a particular concern for people living with HIV, for both people who are not on HIV treatment and those who are, in ensuring they have access to medicines and health facilities.
The COVID-19 pandemic throws into sharp relief existing inequalities, including gender inequality and economic inequality.

In Chamazi, many women make a living selling homemade food, such as buns, fish or ice cream, or selling groceries in small kiosks.
Ms Damiani, a single mother of three, says her business was greatly affected by the COVID-19 pandemic. “Many people no longer wanted to buy my buns or home-made ice cream. I also couldn’t go to the main market to sell because of the crowds and the risk it brought. I then decided to switch completely to selling groceries at a small kiosk and rearing ducks and chickens to sell,” says Ms Damiani.

Ms Damiani has been living with HIV since 1998. All her three children are HIV-negative. Her husband divorced her and married another woman due to her HIV status and pressure from his family. To date, she still does not know his status. She lives with her daughter and granddaughter as her sons each have their own families. Her daily routine now includes feeding her ducks and chickens, helping her granddaughter with her schoolwork, performing household chores and tending her kiosk.

Ms Damiani says the COVID-19 pandemic affected her mental health. “I don’t have many friends and I spend most of my time at home or at the church. My stress levels increased in the earlier days of the pandemic and I began to lose weight,” she says.

“Fortunately, I never stopped taking my HIV treatment due to the insistence of my doctors that I adhere to my treatment regimen,” she says. “I am now determined to show everyone that you can live a full and healthy life as long as you don’t stop taking your medication.”

“The education and support we received from the Hebu Tuyajenge project also greatly helped to alleviate my stress.”
Hebu Tuyajenge is an initiative of the National Council of People Living with HIV, with support from UNAIDS and funded through USAID.
It focuses on increasing the utilization of HIV testing, treatment and family planning services among adolescents and people living with HIV, strengthening the capacity of community organizations and structures and empowering people living with HIV. In the face of the COVID-19 pandemic its members educated people living HIV on how to protect themselves from COVID-19.
“In my community, one of the biggest problems was the lack of education and information surrounding COVID-19. Most of us didn’t even know how to properly wash our hands to reduce the risk of catching the virus,” says Ms Damiani.

The Hebu Tuyajenge project is an example of how the government, development partners, civil society and community activists have been key in responding to COVID-19 in the United Republic of Tanzania, providing information, services, social protection and hope to people living with HIV during these unprecedented and trying times.

“The efforts by the government and other donors should continue. Things have now improved in the country because everyone is now aware of the pandemic and people continue to take precautions,” says Ms Damiani.
Coming together to address the cost of inequality
“My business suffered because of corona. Before corona, I would sell at least 10 egg trays a week. At the height of the pandemic, I was lucky if I could sell two trays,” lamented George Richard Mbogo, who is living with HIV, a father of two, and owns a chicken, egg and chips business in Temeke, a district in the southern part of Dar es Salaam, United Republic of Tanzania.
The COVID-19 crisis has adversely impacted the livelihoods of people living with HIV in the United Republic of Tanzania, exacerbating the challenges they face. These include HIV service delivery and widening social and economic inequalities.
“Corona has been a very difficult time. I lived with a lot of worry and stress. Driving a bodaboda (motorbike taxi) requires going into crowds and working closely with people. It has been difficult not to fall into anxiety and depression, balancing getting my HIV treatment and work. I had moments thinking of stopping taking my meds, but I didn’t,” said Aziz Lai, a motorcycle driver who also lives in Dar es Salaam.
Although the colliding pandemics of HIV and COVID-19 are hitting the poorest and the most vulnerable the hardest, through national resource mobilization the COVID-19 crisis has created an opportunity for partners to mobilize in support of the communities they serve.
The collaborative efforts between the government, development partners, including the United States President’s Emergency Plan for AIDS Relief, USAID and UNAIDS, the National Council of People Living with HIV (NACOPHA) and community activists have been key in responding to COVID-19, providing information, services, social protection and hope to people living with HIV during these unprecedented and trying times.
One such initiative is Hebu Tuyajenge, run by NACOPHA and funded by USAID, which focuses on increasing the utilization of HIV testing, treatment and family planning services among adolescents and people living with HIV, strengthening the capacity of community organizations and structures and improving the enabling environment for the HIV response through empowering people living with HIV.
Caroline Damiani is a single mother of three who is living with HIV and keeps chicken and ducks for a living. “Hebu Tuyajenge gave us personal protective equipment, sanitizers, soap and buckets and education about COVID-19 and how to take care of ourselves in order to stay healthy during the pandemic,” she said.
Through community-based services that supplement facility-based care, people living with HIV have been linked to and kept on treatment during the crisis by critical peer-to-peer HIV services.
For Elizabeth Vicent Sangu, who has been living with HIV for 26 years, her “numbers” speak for themselves.
“From my community follow-ups, I have returned 80 people to the clinic for CD4 count testing, inspired 240 people to get tests, reported 15 gender-based violence cases and provided education to 33 groups, including youth and church groups,” she said, beaming with pride.
NACOPHA helped Ms Sangu to come to terms with her status and helped her on her own journey of self-empowerment.
“Since becoming a treatment advocate for Hebu Tuyajenge, I have received help with entrepreneurship and education about HIV. I have become a teacher for others. I have made others brave about living with HIV and getting tested,” she said.
The partnership between community advocates and health facilities has paid off.
“Both we and our patients were fearful initially, but due to information and education, things got better. We focused on providing hourly and daily information to patients about corona and made sure that people practised safe social distancing,” said Rose Mwamtobe, a doctor at the Tambukareli Care and Treatment Centre in Temeke.
“Not only in the United Republic of Tanzania, but globally, COVID-19 is showing once again the cost of inequality. Global health, including the AIDS response, is interlinked with human rights, gender equality, social protection and economic growth,” said Leopold Zekeng, UNAIDS Country Director for the United Republic of Tanzania.
“The key to ending AIDS and COVID-19 is for all partners to come together, on a country and global level, to ensure that we leave no one behind,” he said.
The shero of Butha-Buthe: Matšeliso Setoko
Matšeliso Setoko stands at the gates of Seboche Mission Hospital in Lesotho and points at the high mountain peaks in the distance.

“Some of our patients come from beyond those mountains,” she says. “Some of them will walk for two hours before they find a taxi, then will ride in the taxi for another three hours before they get here. Some come on horseback.”

Seboche Hospital is located in Butha-Buthe, Lesotho’s northernmost district, in the village of Ha Seboche, accessible only via a winding dirt road with steep twists and turns. Despite its remote location, the hospital has gained a reputation as a centre of excellence since its founding in 1962 and people are willing to travel long distances to go there.

Ms Setoko is the head of the hospital’s antiretroviral therapy clinic and frequently goes out of her way to ensure that her patients have access to their medicines and adhere to their treatment. Lesotho has the second highest HIV prevalence in the world, with an estimated 340 000 people living with HIV. Twelve thousand are children between the ages of 0 and 14 years.
“We often encounter difficult cases,” she explains. “For example, some children have lost their parents, are diagnosed HIV-positive and are chased out of their relatives’ homes when their relatives find out about the diagnosis. In those cases, I go and talk to the relatives to try and understand why they would do such a thing. I find out who the child’s new treatment supporter is and I work closely with him or her to make sure that the child continues to take their medication.”

The arrival of COVID-19 in Lesotho, however, brought a set of challenges unlike anything that Ms Setoko has faced in her 23 years of working at Seboche Hospital.

In the first week of July 2020, a staff member tested positive for COVID-19 and the hospital was forced to shut down for a week. This coincided with the beginning of a nationwide strike by health workers, who demanded that the government provide them with a COVID-19 risk allowance and adequate personal protective equipment. The strike only ended on 27 July.

“Our services were suspended for most of July, but I knew that I had to find a way to help my patients, particularly the children I work with,” says Ms Setoko. “I’m responsible for about 130 children who are on HIV treatment. So, I went to the filing cabinets and took out all their files and found out that many of them needed refills. I went to the pharmacy and got the medication for all of them—enough for three months.”
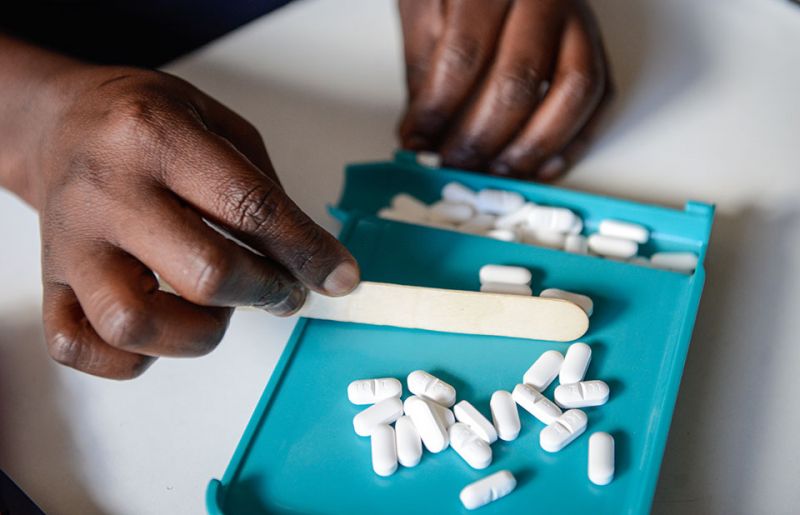
Ms Setoko then liaised with her colleagues—lay counsellors, nurses and other staff members—to find out who lived in the same villages as her patients. She assembled packages of medicines for each village and asked her colleagues to take them home. She then called all the children’s carers to inform them that their medicine could be picked up from the hospital staff member living in their village.
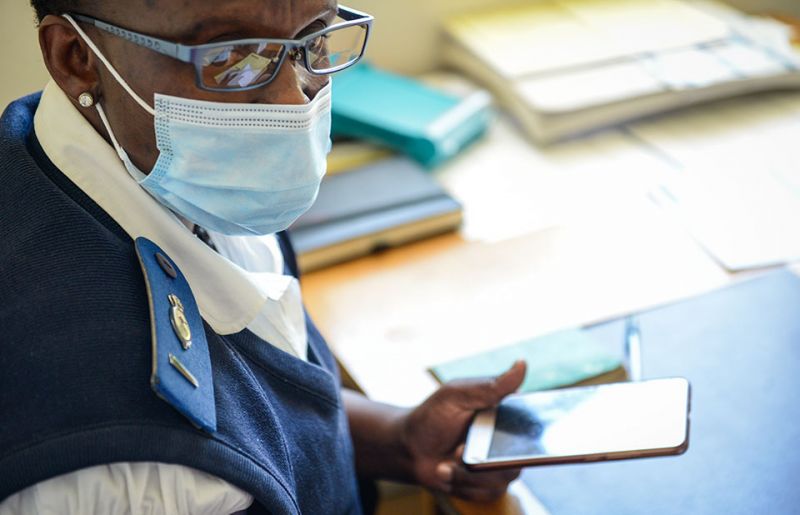
Due to COVID-19 travel restrictions, the borders between Lesotho and South Africa were closed from the end of March to the beginning of October. Many of Ms Setoko’s adult patients are migrant workers in South Africa. Before the onset of COVID-19, her patients would regularly travel from South Africa back to Seboche Hospital to collect their three months’ worth of HIV treatment or would send a relative to pick up their medicine on their behalf. With borders closed, however, many found themselves stuck in South Africa for six months. Again, Ms Setoko had to devise innovative solutions to ensure that her patients did not default on their treatment.

“I think I helped around 50 patients who were in South Africa,” she recalls. “If they were about to run out of antiretroviral therapy, I asked them to identify the clinic closest to them and wrote a referral letter for them. I then took a picture of the letter and sent it to them via WhatsApp or else emailed a PDF copy of the letter to the clinic if that was required. I would also call the nurses at the relevant clinic in South Africa to make sure that my patients received the correct antiretroviral medicines.”
There is a low rate of testing for COVID-19 in Lesotho, with less than 2% of the country’s population having been tested.
“The numbers we are seeing do not give us a true picture of what is happening with COVID-19 in this country,” sighs Ms Setoko. “We are not doing enough testing and it can take weeks for people to get their results. We are also not doing enough contact tracing, so it makes it difficult to contain the spread of the virus.”
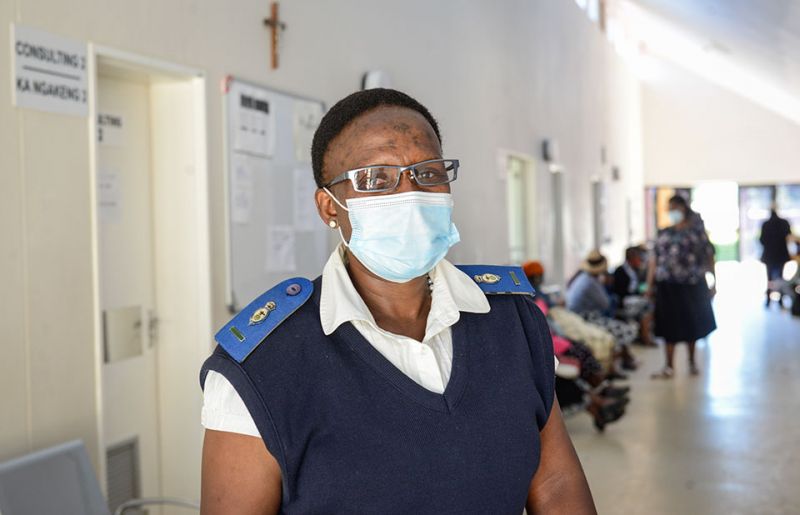
In the face of such challenges, Ms Setoko recognizes the value of cooperation and solidarity, both at the community and organizational levels, in efforts to continue with HIV prevention and treatment programmes in the era of COVID-19.
“As Seboche Hospital we are lucky to have the support of other organizations, such as our strong partnership with SolidarMed, a Swiss non-profit organization. We also work closely together as staff from different departments, because when people work together, they can achieve any goal.”
HIV community activists tackle COVID-19 in Lesotho
It is a sunny weekday morning in the small town of Morija, Lesotho. On the expansive lawn of the Morija Museum and Archives, under the shade of tall trees, a group of children and teenagers sit on evenly spaced plastic chairs.
They have all had their temperatures checked, have washed their hands at purpose-built tippy-taps and are wearing brightly coloured seshoeshoe fabric face masks.
The learners would usually be in school at this time, but schools throughout the country remain closed due to COVID-19. In response to this crisis, local community-based organizations have had to implement new and innovative programming.
This particular programme is called Skills & Soup, implemented by the Hub, a Morija-based nongovernmental organization. On a bi-weekly basis, groups of learners visit to receive a nutritious meal and participate in a range of activities and educational programming, including dance and taekwondo, maths and science lessons and COVID-19 awareness sessions.
Today, the Hub is hosting a pair of guest facilitators from the Maseru-based nongovernmental organization Kick4Life, which specializes in delivering HIV and life skills education through sports-based curricula.
Puky Ramokoatsi, an experienced educator and gender equality activist, is leading the session with confidence and ease. She begins with an energizer, getting the learners to stand up to chant and dance along with her, all the while remaining at a two-metre distance from one another. She keeps her mask on throughout the session, the volume and authority of her voice unhindered.
During the session, Ms Ramokoatsi and her co-facilitator, Mbulelo Mochochoko, play a series of sound clips from a portable speaker. The clips, taken from new animations developed by Kick4Life, feature catchy music and short conversations between two characters who discuss a range of health-related topics, including HIV, nutrition, mental health and ways to protect oneself against COVID-19.
“Who can remind me which fluids can transmit HIV?” asks Ms Ramokoatsi after one of the clips has played. The children stand up and stretch their hands out eagerly, competing to be the first to give the correct answer.
The session is a far cry from Kick4Life’s signature programming, which typically includes close-contact games and activities, with children huddled in groups for discussions or holding hands while standing in a circle.
As with community-based organizations across the region, Kick4Life has adapted its approach to HIV and health education to mitigate the risk of COVID-19 transmission and in response to national lockdowns and government-mandated restrictions.
“We were forced to close our offices in March, when Lesotho went into lockdown, so we had to quickly adjust,” Ms Ramokoatsi explains. “We partnered with the British High Commission in Lesotho to adapt our curriculum into six short animations which could be easily distributed through our online platforms and to include new messaging about COVID-19. We also aired the sound clips from these animations on national radio stations. These are some of the ways that we continued to engage with young people even during the lockdown.”
While COVID-19 cases remain relatively low in Lesotho, at just over 2000 cumulative cases as of November 2020, testing capacity is also low. Only 25 500 tests have been conducted since March 2020. By comparison, a neighbouring country, South Africa, has conducted more tests than this in one day.
In 2019, there were 340 000 people living with HIV in Lesotho, 120 000 of whom are not on HIV treatment.
In addition, a third and silent epidemic plagues Lesotho—that of sexual and gender-based violence. It is estimated that one in three women in Lesotho have experience sexual or physical violence in their life—the same as the global average.
Ms Ramokoatsi has been involved with Kick4Life since 2010, when she began to participate in the organization’s programmes because of her love for football. At the time, she knew very little about HIV, and her interest in the issue was piqued by the fact that her aunt had recently died of AIDS-related illnesses.
“I didn’t understand enough about HIV when my aunt was sick,” recalls Ms Ramokoatsi. “I judged her negatively and didn’t support her. When I learnt more about HIV, I realized how wrong I had been. I made it my purpose after that to support people living with HIV, to give others the support that I hadn’t given my aunt.”
Having experienced sexual abuse herself, Ms Ramokoatsi is acutely aware of the healing power of sports and education and reflects on the difficult transition from face-to-face learning and close-contact activities to virtual and socially distanced programming.
“Before COVID-19 we were in the process of helping several young women who had experienced sexual violence and were slowly opening up to us after taking part in our programmes,” Ms Ramokoatsi explains. “When we were forced to close, we lost touch with some of them. We’ve had to find ways to continue with our programmes and to keep reaching out to our participants, but it hasn’t been easy.”
Ms Ramokoatsi emphasizes the importance of organizations working together in their responses to COVID-19 awareness and health education. “Today, for example, we’re delivering this session thanks to our partnerships,” she says. “I hope more organizations can work like this to share resources and information.”
“I always say that the best part of the game is the opportunity to play. That attitude applies to everything: instead of sitting on the sidelines, get involved. Learn about the situation or the issues around you, whether it’s HIV or gender-based violence or COVID-19. Learn how you can adapt, how you can take care of yourself, and then find a way to help others,” she says.
More...
YOUNG PEOPLE, SEXUAL AND REPRODUCTIVE HEALTH AND COVID-19
On 12 August 2020, the world united in its commemoration of International Youth Day. This year’s theme, Youth Engagement for Global Action, highlights how the engagement of young people enriches national and multilateral institutions and processes. It also draws attention to how their representation and engagement in formal institutional politics can be significantly enhanced.
2020 has been marked by the COVID-19 pandemic, which aggravates many of the challenges faced by young people in Africa, including lack of access to integrated HIV, sexual and reproductive health and rights (SRHR) and gender-based violence (GBV) information, services and commodities, loss of livelihoods and education opportunities.
It is against this background that UNAIDS Regional Support Team for Eastern and Southern Africa, in partnership with the SADC Parliamentary Forum (SADC-PF), UNFPA, UNESCO, Restless Development, AfriYAN and the African Population and Health Research Centre, have joined forces in convening a series of online engagements with Speakers of National Parliaments, parliamentarians and young people in all their diversity.
Now more than ever, decision-makers, including parliamentarians, need to be informed about the specific needs of young people to take adequate measures into response and recovery plans.
“We must infuse urgency into implementation when we have heard from young people, so that we accelerate our responsiveness to their conditions”, said the Deputy Speaker of the National Assembly of South Africa, Solomon Lechesa Tsenoli, in his remarks during the webinar convened on 12 August 2020 in commemoration of International Youth Day.
The webinar series seeks to advance the commitments set out in the ground-breaking Tshwane Declaration, adopted by SADC-PF Assembly in December 2019, building on the outcomes of a regional Youth Indaba that same year. The Tshwane Declaration focuses on the domestication, harmonization and implementation of laws and policies concerning young people’s SRHR.
“My belief is that if we work very hard as a country, in a time not very far away from us, we should have recognized different definitions of children’s laws in this country”, said the Deputy Speaker of the National Assembly of Botswana, Mabuse Mopati Pule, about providing a clear age of consent to health care services in legislative provisions for the benefit of adolescents and service providers.
The engagements provide a unique platform for young people to share experiences, ideas, and possible solutions with decision-makers with the goal to strengthen young people’s ability to exercise accountability, while advocating for the fulfilment of their right to health and education.
“We do often say, nothing about us, without us. As young leaders we need to carry this statement as we seek political spaces and voice the needs of our fellow young people,” said Hussein Melele, Vice-President of AfriYAN Eastern and Southern Africa.
“The youth can influence incremental change and the interface between youth and parliaments can bring enhancement towards social transformation in the field of SRHR. The relevance of youth in relation to implementation of SRHR cannot be overemphasized, given that it is the youth that are primarily affected by issues such as lack of contraception and safe abortion”, said the Secretary General of the SADC Parliamentary Forum, Boemo Sekgoma, in her introductory remarks.
THE IMPACT OF COVID-19: LESSONS FROM THE AIDS RESPONSE
As the world scales up public health responses to the COVID-19 pandemic, countries are being urged to take decisive action to control the epidemic with containment and service provision as central pillars.
However, as in all acute epidemics, especially where person-to-person transmission occurs, there is a need to ensure that the response is grounded firmly in human rights and that the vulnerability of certain groups is not exacerbated, including women and girls.
The UNAIDS Regional Support Team for Eastern and Southern Africa recently co-hosted a high-level webinar with the Southern African Development Lawyers’ Association (SADC-LA) to discuss the challenges faced in the region due to the COVID-19 pandemic and its implications for social justice, human rights and gender-based violence.
“A primary lesson from the HIV response is that restrictive, stigmatizing and punitive measures can lead to significant human rights abuses. These come with disproportionate effects on already vulnerable communities, including key populations”, said Aeneas Chuma, interm Director of the UNAIDS Regional Support Team for Eastern and Southern Africa, in his opening remarks.
Mr Chuma recommended an approach that moves away from compulsory restrictions towards a focus on reaching and serving those who are most vulnerable, empowering people with knowledge and tools to protect themselves and others, and the removal of barriers. These are lessons learnt from the AIDS response, he said.
Across the region governments have declared states of emergencies and enforced restrictions to tackle the COVID-19 pandemic. In many instances this has been followed by reports on increased violations of human rights and police brutality.
“We need vigilance in ensuring that the restrictions of human rights in the quest of saving lives does not become an incentive to undermine the rule of law and increase violence. We need to pursue advocacy with respect to the vulnerability of women, LGBTQ people and sex workers during this period,” said Maxwell Xolani Boqwana, President SADC-LA.
One of the main aims of the webinar was to provide practical and substantive guidance to policy makers on the best ways to preserve human rights and the rule of law in the wake of COVID-19.
In her remarks, Yvonne Dausab, Minister of Justice Namibia, cited examples on how this has been tackled in Namibia.
“In Namibia, the state of emergency is provided for by the Supreme Court under the Constitution which was further approved by the National Assembly. An additional safeguard is the fact that the various agencies and ministries had to provide directives on how to manage the state of emergency,” she said.
With the spread of COVID-19, cases of gender-based violence (GBV) have increased substantially, especially in the eastern and southern Africa region where such violence is already widespread.
“In times of crises the gap between rich and poor increases, women are at the core of any negative impact. Most gender-based violence happens at home, meaning that women are locked down with abusers in a way that threaten their lives. As parliamentarians we have the mandate to make legislation and hold governments accountable to adopt measures on prevention and support,” said Sylvia Mthethwa, Senator of Eswatini and Member of the Pan-African Parliament.
Some measures that have been put in place to protect women and children from violence include government hotlines, support to shelters (Zambia), free 24-hour emergency medical services (Kenya), and mobile GBV clinics (Mozambique).
“Malawi faces similar challenges to many other African countries. How are we supposed to carry out lockdown and practice social distancing in a context where people lack the preventative measures to spread this pandemic? We see worrying parallels with the HIV epidemic, including stigma and lack of access to information and the intersectional vulnerabilities of women and girls.,” said Sarai Chisala Tempelhof, Executive Director of the Gender Justice Unit in Malawi.
The platform will reconvene, with engagement from more stakeholders to continue sharing information on shaping the COVID-19 response, taking into consideration its implications on human rights, social justice and GBV.
“This is a new normal and it is not going to go away, we have to embrace change and bring on innovation. We need to look at how to scale up good practices. We have to integrate the COVID-19 response with existing work on tackling HIV and GBV,” said Alti Zwandor, UNAIDS Country Director in Namibia.
Talking about a revolution
It is no surprise that Birknesh Teferi’s first name means “revolution” in Amharic, the language spoken in Ethiopia. She exudes passion and self-pride; she’s the picture of health and well-being.
Her journey to this point in her life is indeed revolutionary—a story of resilience, hope and transformation. She has beaten tuberculosis (TB), survived cervical cancer and is living positively with HIV.
Ms Teferi was diagnosed with HIV and TB in 2003, a time when information about HIV, TB and sexual and reproductive health in Ethiopia was scarce and stigma and discrimination high.
According to the World Health Organization (WHO), Ethiopia is one of the 48 high-burden TB countries globally. In 2018 in the country, 165 000 people fell ill with TB and there were 27 000 deaths; 2200 of which were among people living with HIV.
After waiting 15 days for her test results, while the health-care worker went on leave, Ms Teferi was told that she was “positive”.
“I thought it was good news. I hugged the nurse in relief, only for her to tell me that being HIV-positive meant I had the virus,” she said.
Ms Teferi successfully underwent the WHO recommended treatment for TB—directly observed treatment short-course (DOTS)—which cured the TB but did not help her with her struggle to accept her HIV status.
“What followed was a period of hurt and heartbreak … Waiting for death,” she recalled of the aftermath of her diagnosis.
She describes herself then as a “drifter.” She did not disclose her HIV status because of stigma and worked as a sex worker to make ends meet.
“If a client had a condom, we would use it. If he didn’t, we didn’t. I tried to use them, but I had no money to buy them. That’s how I developed a sexually transmitted infection.”
During the treatment of the infection, Ms Teferi was diagnosed with cervical cancer and was referred from one health facility to the next, often in different towns.
She eventually found a “caring” doctor and had an operation to treat the cancer. “I was in so much pain, I couldn’t sit. I was miserable,” she remembers.
But when Ms Teferi started to take HIV treatment in 2008, her life slowly changed. She started to look after herself more. She insisted on condom use with her clients.
She met a group of women living with HIV from the Tilla Association of HIV-Positive Women in Hawassa, Ethiopia. The association focuses on capacity-building and training and support of women living with HIV. It runs an embroidery centre as an income-generating activity for women living with HIV, where Ms Teferi now works.
“I am now free of drifting. Life is so much better. If people feel that it is possible to live, possible to work, then life can change,” she said.
For the first eight months of her time at the centre, the manager assigned her a volunteer to help her with her physical recovery from her operation. For the first time, she had support from other women who understood what it was like to be her.
The women at the centre invited her to watch a film about living positively with HIV. “That movie gave me hope,” she says. “I started to learn more about HIV from my manager. I gradually got relief, better medical services and Tilla supported me financially and emotionally.”
While Ms Teferi is on HIV treatment and has been cured of TB, there are millions of people worldwide who still lack access to prevention and treatment for both conditions. TB is the leading cause of death among people living with HIV globally.
In 2018, there were an estimated 1.2 million TB deaths, 251 000 of which were among people living with HIV—this is a 60% reduction from 620 000 in 2000. Between 2000 and 2018, TB treatment alone averted an estimated 48 million deaths among HIV-negative people and TB treatment supported by antiretroviral therapy averted an additional 10 million deaths. However, progress is slow and needs to be accelerated in order to end TB by 2030 as part of the Sustainable Development Goals.
“TB is curable and preventable,” said Aeneas Chuma, the Director for the UNAIDS Regional Support Team for Eastern and Southern Africa, a.i. “It is critical in this moment of history, in the context of the global COVID-19 pandemic, that we ensure that people living with HIV who are diagnosed with TB have uninterrupted access to HIV and TB treatment. UNAIDS is working with governments and community partners to ensure that we adapt to a rapidly changing health context, with kindness, compassion and humanity.”
Living with HIV under lockdown
Pumza Mooi is worried. A resident of Port Elizabeth, South Africa, she is one of 2.5 million people in the country living with HIV but not currently on antiretroviral therapy.
“I’ve decided that I have to start,” said Ms Mooi. “No matter how strong my CD4 count or how low my viral load, it will never be as good as on HIV treatment. It is something I must do for myself, for my children and for those who look up to me. I am scared of getting sick,” she said.
Ms Mooi’s decision to start HIV treatment comes at a time of uncertainty for people with a compromised immune system, owing to the risk of a severe COVID-19 infection. There is currently no evidence that people living with HIV have any greater risk of acquiring COVID-19, but there is concern that a COVID-19 infection could be more severe for people living with HIV who are not taking antiretroviral therapy.
South Africa is under a 21-day lockdown to try to slow the spread of COVID-19 and Minister of Health Zweli Mkhize has urged everyone to take precautions to prevent infection, emphasizing the importance of everyone knowing their HIV status, getting tested and immediately starting treatment should they test positive.
“The thought of catching COVID-19 frightens me,” said Ms Mooi. “It is scary to think that I already have one virus [HIV] that my body is dealing with. I am asking myself, is my body strong enough, is my immune system strong enough?”
Ms Mooi acquired HIV many years ago, when the prevailing advice was to commence treatment if the patient experienced a reduction in their CD4 count, thus falling ill. She has been monitoring her status ever since. In 2016, the World Health Organization published new guidelines recommending lifelong antiretroviral therapy for all children, adolescents and adults, including all pregnant and breastfeeding women living with HIV, regardless of their CD4 cell count. In other words, anybody diagnosed with HIV should start treatment straight away.
UNAIDS is actively monitoring the impact of COVID-19 and working with networks of people living with HIV, the government and development partners to ensure that the concerns of people living with HIV are heard and reflected in the COVID-19 response. This includes identifying constraints on health services, encouraging longer, multimonth prescriptions of antiretroviral medicine and helping communities to provide solutions.
Social networking
Life under lockdown is especially difficult for people living in informal settlements and UNAIDS has recognized the challenge of achieving self-protection, social distancing and containment in such areas. Added to this are fear-inducing and inaccurate reports about the coronavirus. “There is a lot of information going around but not all of it is true,” Ms Mooi said. “I am reminding people that the government has given us a WhatsApp number where we can get good information, and not to worry about other information. If it is true, the government will tell us.”
Luckily, Ms Mooi has a robust support network after she shared her HIV status online many years ago. “I know I will be looked after,” she says. She moderates Facebook and WhatsApp support groups for people living with HIV that have dozens of members, ranging in age from a 16-year-old born with HIV to a woman of 62 who has lived with HIV for many years.
Over the past few years, many in the group have shared their experiences of living with HIV and their experiences of taking HIV treatment, confronting stigma and discrimination and staying motivated. Their consensus is that taking and adhering to HIV treatment is the best option, Ms Mooi said.
Right now, there is a new topic in the groups. “They are worried about COVID-19,” Ms Mooi said. “I tell them don’t worry, stay home and practice good hygiene.” For the time-being, everyone knows they will have to sit tight and take care of each other remotely, to get through extended isolation.
The group fosters discussion mostly among women, although men are listening in. “I get messages from men asking why we don’t discuss issues affecting them, but if they don’t disclose they won’t always get the help they need,” she says. “I encourage men to share their stories and let us help each other.”
Looking ahead
Like most, Ms Mooi is already looking forward to being able to move about more freely again and to start HIV treatment. She is doing what she can to look after her family and to encourage her networks of people living with HIV. “We are doing the things we are told to do, like washing our hands and keeping away from other people, and just praying and hoping for the best,” she said.




















